1. You find an unresponsive patient who is not breathing. After activating the emergency response system, you determine that there is no pulse. What is your next action?
A. Open the airway with a head tilt–chin lift.
B. Administer epinephrine at a dose of 1 mg/kg.
C. Deliver 2 rescue breaths each over 1 second.
D. Start chest compressions at a rate of at least 100/min.
2. You are evaluating a 58-year-old man with chest pain. The blood pressure is 92/50 mm Hg, the heart rate is 92/min, the nonlabored respiratory rate is 14 breaths/min, and the pulse oximetry reading is 97%. What assessment step is most important now?
A. PETCO2
B. Chest x-ray
C. Laboratory testing
D. Obtaining a 12-lead ECG
3. What is the preferred method of access for epinephrine administration during cardiac arrest in most patients?
A. Intraosseous
B. Endotracheal
C. Central intravenous
D. Peripheral intravenous
4. An activated AED does not promptly analyze the rhythm. What is your next action?
A. Begin chest compressions.
B. Discontinue the resuscitation attempt.
C. Check all AED connections and reanalyze.
D. Rotate AED electrodes to an alternate position.
5. You have completed 2 minutes of CPR. The ECG monitor displays the lead II rhythm below, and the patient has no pulse. Another member of your team resumes chest compressions, and an IV is in place. What management step is your next priority?
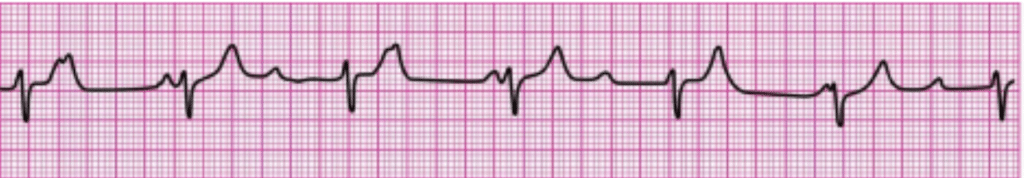
A. Give 0.5 mg of atropine.
B. Insert an advanced airway.
C. Administer 1 mg of epinephrine.
D. Administer a dopamine infusion.
6. During a pause in CPR, you see this lead II ECG rhythm on the monitor. The patient has no pulse. What is the next action?
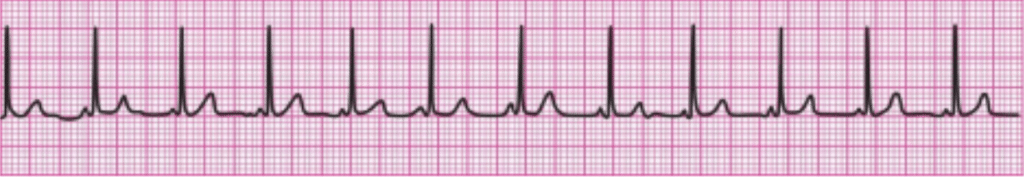
A. Establish vascular access.
B. Obtain the patient’s history.
C. Resume chest compressions.
D. Terminate the resuscitative effort.
7. What is a common but sometimes fatal mistake in cardiac arrest management?
A. Failure to obtain vascular access
B. Prolonged periods of no ventilations
C. Failure to perform endotracheal intubation
D. Prolonged interruptions in chest compressions
8. Which action is a component of high-quality chest compressions?
A. Allowing complete chest recoil
B. Chest compressions without ventilation
C. 60 to 100 compressions per minute with a 15:2 ratio
D. Uninterrupted compressions at a depth of 1½ inches
9. What should be done to minimize interruptions in chest compressions during CPR?
A. Perform pulse checks only after defibrillation.
B. Continue CPR while the defibrillator is charging.
C. Administer IV medications only when breaths are given.
D. Continue to use AED even after the arrival of a manual defibrillator.
10. Which condition is an indication to stop or withhold resuscitative efforts?
A. Unwitnessed arrest
B. Safety threat to providers
C. Patient age greater than 85 years
D. No return of spontaneous circulation after 10 minutes of CPR
11. After verifying the absence of a pulse, you initiate CPR with adequate bag-mask ventilation. The patient’s lead II ECG appears below. What is your next action?
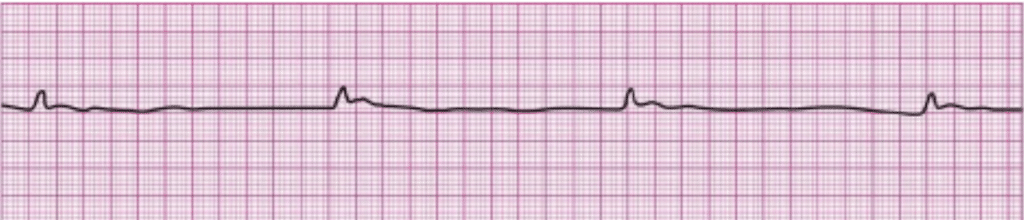
A. IV or IO access
B. Endotracheal tube placement
C. Consultation with cardiology for possible PCI
D. Application of a transcutaneous pacemake
12. After verifying unresponsiveness and abnormal breathing, you activate the emergency response team. What is your next action?
A. Retrieve an AED.
B. Check for a pulse.
C. Deliver 2 rescue breaths.
D. Administer a precordial thump.
a. start fibrinolytic therapy ASAP
b. hold fibrinolytic therapy for 24 hours
c. order an echo before fibrinolytic administration
d. wait for MRI result
For STEMI pt, maximum goal time for ED door-to-balloon-inflation time for PCI?
a. 150 mins
b. 180 mins
c. 120 mins
d. 90 mins
Which is the recommended oral dose of aspirin for a patient with suspected acute coronary syndrome?
a. 81 mg
b. 325-650 mg
c. 160-325 mg
d. 40 mg
chest compressions during for adult rate
a. 40-60/min
b. 60-80/min
c. 80-100/min
d. 100-120/min
What is the effect of excessive ventilation?
a. decresed cardiac output
b. decreased intrathoracic pressure
c. increased perfusion pressure
d. increased venous return
temperature to achieve targeted temperature management after cardiac arrest
a. 30-34C
b. 32-36C
c. 36-40C
d. 38-42C
3 mins into cardiac arrest resuscitation attempt, one member of your team inserts an endotracheal tube while another performs chest compressions. Capnography shows a persistent waveform & a PETCO2 of 8mmHg. What is the significance of the finding?
a. chest compression may not be effective
b. The endotrachael tube is in the esophagus
c. the team is ventilating the patient too often
d. the patient meets the criteria for termination of efforts
Your patient is in cardiac arrest and has been intubated. To assess CPR quality, you should?
a. obtain a chest x-ray
b. check the patient’s pulse
c. monitor the patient’s PETCO2
d. obtain a 12-lead ECG
In addition to clinical assessment, which is the most reliable method to confirm & monitor correct placement of an endotracheal tube?
a. arterial blood gas
b. hemoglobin levels
c. chest radiography
d. continuous waveform capnography
A 45M had coronary artery stents placed 2 days ago. Today he is in severe distress and reporting “crushing” chest discomfort. He is pale, diphoretic, and cool to the touch. His radial pulse is very weak, blood pressure is 64/40, respiratory is 28 bpm/min and O2 set is 89% on room air. When applied, the cardiac monitor initially showed ventricular tachycardia, which then quickly changed to ventricular fibrillation.
WhIn addition to defibrillation, which intervention should be performed immediately?
a. chest compression
b. vasoactive meds
c. vascular access
d. advanced airway
A 45M had coronary artery stents placed 2 days ago. Today he is in severe distress and reporting “crushing” chest discomfort. He is pale, diphoretic, and cool to the touch. His radial pulse is very weak, blood pressure is 64/40, respiratory is 28 bpm/min and O2 set is 89% on room air. When applied, the cardiac monitor initially showed ventricular tachycardia, which then quickly changed to ventricular fibrillation.
Despite 2 defibrillation attempts, the patient remains in V-fib. Which drug and dose should you administer?
a. lidocaine 1 mg/kg
b. amiodarone 300mg
c. epinephrine 1mg
d. atropine 1 mg
A 45M had coronary artery stents placed 2 days ago. Today he is in severe distress and reporting “crushing” chest discomfort. He is pale, diphoretic, and cool to the touch. His radial pulse is very weak, blood pressure is 64/40, respiratory is 28 bpm/min and O2 set is 89% on room air. When applied, the cardiac monitor initially showed ventricular tachycardia, which then quickly changed to ventricular fibrillation.
Despite the drug provided above and continued CPR, the patient remains in v-fib. Which drug should be administered next?
a. atropine 1mg
b. mag sulfate 1g
c. amiodarone 300mg
d. epi 1 mg
A 45M had coronary artery stents placed 2 days ago. Today he is in severe distress and reporting “crushing” chest discomfort. He is pale, diphoretic, and cool to the touch. His radial pulse is very weak, blood pressure is 64/40, respiratory is 28 bpm/min and O2 set is 89% on room air. When applied, the cardiac monitor initially showed ventricular tachycardia, which then quickly changed to ventricular fibrillation.
The patient has return of spontaneous circulation and is not able to follow commands. Which immediate post-cardiac arrest care intervention do you choose for the patient?
a. extubate
b. check the glucose level
c. administer epinephrine
d. initiate targeted temperature management
A 45M had coronary artery stents placed 2 days ago. Today he is in severe distress and reporting “crushing” chest discomfort. He is pale, diphoretic, and cool to the touch. His radial pulse is very weak, blood pressure is 64/40, respiratory is 28 bpm/min and O2 set is 89% on room air. When applied, the cardiac monitor initially showed ventricular tachycardia, which then quickly changed to ventricular fibrillation.
Which would you have done first if the patient had not gone into ventricular fibrillation?
a. given atropine 1mg
b. established IV access
c. obtained a 12 lead
d. performed synchronized cardioversion
During post-cardiac arrest, which is recommended duration of targeted temp. management after reaching the correct temperature range?
a. at least 24 hours
b. 0-8 hour
c. at least 36 hours
d. at least 48 hours
which is the primary purpose of medical emergency team or rapid response team?
a. provide diagnostic consultation to emergency department patients
b. provide online consultation to EMS personnel
c. improving patient outcomes by identifying & treating early clinical deterioration
d. improving care for patients admitted to critical care units
Which of these tests should be performed for a patient with suspected stroke within 25 mins of hospital arrival?
a. coagulation studies
b. cardiac enzymes
c. noncontrast CT scan of the head
d. 12 lead ECG
Which of the following signs are likely indicator of cardiac arrest in an unresponsive patient?
a. slow, weak pulse rate
b. cyanosis
c. irregular, weak pulse
d. agonal gasps
Which is the recommended next step after a defibrillation attempt?
a. check the ECG for evidence of a rhythm
b. determine if a carotid pulse is present
c. resume CPR, starting with chest compressions
d. open the patient’s airway


wide complex (monophasic) tachycardia




to properly ventilate a patient w/ perfusing rhythm, how often do you squeeze the bag?
a. once every 10 seconds
b. once every 5 to 6 seconds
c. once every 3 to 4 seconds
d. once every 12 seconds
Which is the recommended 1st IV dose of amiodarone for a patient w/ refractory ventricular fibrillation?
a. 150 mg
b. 250 mg
c. 300 mg
d. 100 mg
Which best describes the length of time it should take to perform a pulse check during BLS assessment?
a. 1 to 4 seconds
b. 5 to 10 seconds
c. 11 to 15 seconds
d. 16 to 20 seconds
If a team member is about to make a mistake during a resuscitation attempt, which best describes the action that the team leader or other team members should take?
a. address the team member immediately
b. conduct a debriefing after the resuscitation attempt
c. remove the team member from the area
d. reassign the team members
As a team leader, when do you tell the chest compressors to switch?
a. about every 2 minutes
b. about every 5 minutes
c. only when they tell you that they are fatigued
d. about every 7 minutes
(I think I put Bag valve mask for this and I got it wrong)
More answers on AHA tests.



